Selective serotonin reuptake inhibitor
This page has not been fully approved by the PsychonautWiki administrators. It may contain incorrect information, particularly with respect to dosage, duration, subjective effects, toxicity and other risks. It may also not meet PW style and grammar standards. |
Selective serotonin reuptake inhibitors (commonly abbreviated as SSRIs) are a class of pharmaceutical antidepressant medications. They are commonly prescribed for the treatment of major depressive disorders. Other conditions include anxiety disorders, obsessive-compulsive disorder, migraine, attention-deficit hyperactivity disorder (ADHD), addiction/dependence, and sleep disorders. The exact pharmacological mechanism of action of SSRIs is unknown.[1] They are believed to increase the extracellular level of the neurotransmitter serotonin, eventually leading to improved mood.[citation needed][clarification needed]
SSRIs can be dangerous when used in combination with other substances that increase or modulate serotonin such as MDMA and Monoamine Oxidase Inhibitors (MAOIs). A combination with these substances can lead to serotonin syndrome and potentially be fatal. SSRIs do not work for everyone and take 3-6 weeks to start having noticeable effects.[2]
SSRIs are reported to have fewer side effects than older antidepressants like monoamine oxidase inhibitors and tricyclic antidepressants.[citation needed] Monoamine oxidase inhibitors also interact with many other medications and foods, leading to a hypertensive crisis that can potentially be fatal. SSRIs can cause sexual dysfunction and compulsive yawning as side effects. Discontinuation of SSRIs can lead to withdrawal symptoms which include flu-like symptoms, as well as brain zaps.
Mechanism of action
SSRIs are believed to increase the extracellular level of the neurotransmitter serotonin by limiting its reuptake into the presynaptic cell, increasing the level of serotonin in the synaptic cleft available to bind to the postsynaptic receptor. They have varying degrees of selectivity for the other monoamine transporters. Pure SSRIs show only weak or negligible affinities for the noradrenaline and dopamine transporters.
SSRIs also lead to an increased level of cAMP (cyclic adenosine monophosphate), BDNF (brain-derived neurotrophic factor), and several other regulatory neuromodulators. Different SSRIs have different binding profiles, leading to slightly different effects.[3]
Subjective effects
Physical effects 
-
- Sedation or stimulation - Some SSRIs are sedating (paroxetine and fluvoxamine), whereas some are mildly stimulating (sertraline and fluoxetine).
- Physical fatigue
- Appetite enhancement or appetite suppression
- Decreased libido - Decreased libido and sexual dysfunction are among the most commonly reported side effects of SSRIs. In some cases these effects may persist after use is discontinued, this is known as PSSD.[4] On the other hand, suppression of depression may enhance libido.
- Orgasm depression - This effect is dose-dependent and causes delayed orgasm, but in some people, especially older users, SSRIs can make one completely unable to reach orgasm. This is usually treated by either switching to a different antidepressant, or adding an NDRI such as bupropion. Short-acting SSRIs such as dapoxetine are approved drugs for premature ejaculation.
- Pain relief - Some studies suggest they can be effective as analgesics (painkillers).[5]
- Nausea - Nausea is mild and is usually only present upon first introduction and usually subsides after 6-8 weeks.
- Headaches - Headaches are usually only present upon first introduction and usually subside after 6-8 weeks.
- Pupil dilation
- Physical fatigue
- Increased perspiration
- Dry mouth
- Vasoconstriction[citation needed]
Visual effects 
-
SSRIs are capable of inconsistently inducing changes in visual perception - often during the beginning of treatment.
Most effects often disappear after a few weeks of treatment but may reappear or become more prominent when combined with cannabis or amphetamines.
Enhancements
- Visual acuity enhancement
- Colour enhancement - this effect is relatively mild but well pronounced.
Distortions
- Tracers
- Drifting (melting, breathing, morphing and flowing) - This effect is most similar in presentation to the same effect from amphetamines but with a cartoony quality most reminiscent of psychedelics such as 4-HO-MET and 2C-B
Hallucinatory states
- Peripheral information misinterpretation - This often manifests itself as seeing minor movement in the corner of one's eye in the absence of any real stimuli.
Cognitive effects 
-
- Apathy[6]
- Motivation suppression or Motivation enhancement - Lack of motivation is anecdotally reported with SSRIs, though on the other hand, suppression of depression or anxiety may enhance motivation.
- Anxiety suppression
- Cognitive fatigue
- Focus suppression
- Dream suppression
- Ego inflation
- Emotion suppression - This effect is similar to but less intense compared to the emotion suppression induced by antipsychotics.
- Emotion enhancement - Upon first introduction, some users can experience amplified emotions.
- Mania
- Derealization
Paradoxical effects 
-
These effects are most often experienced upon first introduction and usually subside after a couple of weeks.
- Nausea
- Headache
- Depression
- Anxiety
- Emotion enhancement
- Thought disorganization
- Irritability
- Motivation suppression
- Suicidal ideation[7] - Some users (especially people under the age of 25)[8] experience increase in suicidal and self harming thoughts and behaviors. This effect usually subsides within 6-8 weeks.
- Insomnia
Experience reports
Experience reports can be found here:
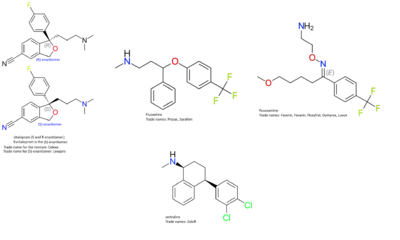
Examples
Citalopram
Citalopram is an SSRI sold under the brand name Celexa in the United States. Citalopram is indicated for the treatment of a major depressive disorder. Citalopram was approved in 1998 by the Food and Drug Administration for the treatment of major depressive disorder.[9] Citalopram is almost exclusively found as the hydrobromide salt, which is the only form approved by the FDA.[10]
Escitalopram
Escitalopram is an SSRI sold under the brand name Lexapro in the United States. Escitalopram is indicated for the treatment of major depressive disorder and anxiety disorders. It is the s-enantiomer of citalopram, and both have similar efficacy. Escitalopram was FDA approved in 2002.[11]
Fluoxetine
Fluoxetine is an SSRI commonly sold under the brand name Prozac. Fluoxetine is indicated for the treatment of major depressive disorder, bulimia nervosa, obsessive-compulsive disorder, panic disorder, and premenstrual dysphoric disorder. Fluoxetine is sometimes used in conjunction with olanzapine (an atypical antipsychotic) to treat bipolar I disorder as well as treatment-resistant depression.[12] A single pill medication called Symbyax is a combination of olanzapine and fluoxetine.[13] Fluoxetine is on the World Health Organization's list of essential medicines, a list of medicines needed for a basic and effective health system.[14] Fluoxetine was first FDA approved in 1987.
Fluvoxamine
Fluvoxamine is an SSRI that is used to treat obsessive-compulsive disorder. Fluvoxamine was first approved by the FDA in 1994.[15] Fluvoxamine has the greatest affinity for the σ1 (sigma-1) receptor, where it acts as an agonist, which may contribute to its biological effects.[16]
Paroxetine
Paroxetine is an SSRI that is sold under the brand name Paxil. Paroxetine is used to treat major depressive disorder, obsessive-compulsive disorder, post-traumatic stress disorder, anxiety disorders, premenstrual dysphoric disorder, and under the brand name Brisdelle, it is used to treat hot flashes related to menopause. Paroxetine was first approved by the FDA in 1992.[17]
Sertraline
Sertraline is an SSRI that is sold under the brand name Zoloft. Sertraline is used to treat major depressive disorder, obsessive-compulsive disorder, post-traumatic stress disorder, anxiety disorders, panic disorder, and premenstrual dysphoric disorder. Sertraline was first FDA approved in 1991.[18]Unlike most SSRIs, sertraline, has notable activity at the dopamine transporter protein[19] and could be considered a serotonin-dopamine reuptake inhibitor.
Other SSRIs
Several other SSRIs have been developed and marketed. Dapoxetine is used in some countries to treat premature ejaculation. Indalpine and zimelidine were originally marketed but later withdrawn due to the emergence of Guillain–Barré syndrome, a serious neurological disease. Cericlamine and panuramine were developed but never marketed.[citation needed]
Drug interactions
A wide array of substances is contraindicated with SSRIs. Substances that increase extracellular serotonin may increase the risk of serotonin syndrome, particularly substances like MDMA, dextromethorphan, tramadol and pethidine. Independent research should be done before taking any substances while on an SSRI to ensure there is no drug interaction. Some dietary supplements such as 5-HTP and St. John's Wort can lead to serotonin syndrome if taken in combination with an SSRI.
Some NSAID analgesics may increase the risk of excess bleeding in those who take SSRIs. NSAIDs include ibuprofen, aspirin (acetylsalicylic acid), and naproxen.
Most SSRIs inhibit the function of certain cytochrome P450 enzymes that metabolize other substances so that SSRIs may lead to an increased or decreased serum level of certain medications.
Combinations
- Psychedelics - Due do the downregulation of 5-HT2A receptors caused by SSRIs, psychedelics can have a reduced effect. SSRIs also reduce the chance of having a bad trip due to its anxiolytic effects.
- Cannabis - The anxiety and paranoia experienced on cannabis may be less intense, or not experienced at all.
- Depressants - SSRIs increase the effects of CNS depressants such as alcohol, opioids, and benzodiazepines. This effect is usually not desired as it may intensify disinhibition and increase the chance of having a blackout.
Dangerous interactions
- Dextromethorphan - Dextromethorphan is a serotonin releaser as well as an SSRI, therefore has a potential to cause serotonin syndrome, a potentially deadly condition caused by extremely high serotonin levels. Although serotonin syndrome caused by this combination is uncommon, it is strongly advised not to combine them, especially if either is at a high dose.
- Empathogens - Combining SSRIs with serotonergic empathogens such as MDMA, mephedrone, and AMT can result in serotonin syndrome.
- Tramadol - Combining SSRIs with tramadol can cause seizures and serotonin syndrome.
- Other antidepressants - Combining SSRIs with other antidepressants such as tricyclic antidepressants and MAOIs can result in serotonin syndrome. Non serotonergic antidepressants such as bupropion are not dangerous to combine with SSRIs.
See also
External links
References
- ↑ http://pi.lilly.com/us/prozac.pdf page 20
- ↑ Do Antidepressants Work Right Away?, 2021
- ↑ Kolb, B., Whishaw, I. Q. (2005). An introduction to brain and behavior (2nd ed ed.). Worth Publishers. ISBN 9780716711872.
- ↑ Pharmacovigilance Risk Assessment Committee (PRAC) (11 June 2019). "New product information wording – Extracts from PRAC recommendations on signals" (PDF). European Medicines Agency. EMA/PRAC/265221/2019.
- ↑ https://www.med.unc.edu/ibs/files/2017/10/IBS-and-Antidepressants.pdf
- ↑ Barnhart, WJ; Makela, EH; Latocha, MJ (May 2004). "SSRI-induced apathy syndrome: a clinical review". Journal of psychiatric practice. 10 (3): 196–9. doi:10.1097/00131746-200405000-00010. PMID 15330228.
- ↑ Björkenstam, C., Möller, J., Ringbäck, G., Salmi, P., Hallqvist, J., Ljung, R. (9 September 2013). "An Association between Initiation of Selective Serotonin Reuptake Inhibitors and Suicide - A Nationwide Register-Based Case-Crossover Study". PLoS ONE. 8 (9): e73973. doi:10.1371/journal.pone.0073973. ISSN 1932-6203.
- ↑ What to know about antidepressants for kids and teens
- ↑ PhD, C. B. N. M. (5 June 2012). Management of Treatment-Resistant Major Psychiatric Disorders. Oxford University Press. ISBN 9780199974146.
- ↑ Citalopram | https://www.drugs.com/citalopram.html
- ↑ Escitalopram | https://www.drugs.com/cdi/escitalopram.html
- ↑ Fluoxetine | https://www.drugs.com/fluoxetine.html
- ↑ Symbyax Prescribing Information | http://pi.lilly.com/us/symbyax-pi.pdf
- ↑ WHO List of Essential Medicines | http://www.who.int/medicines/publications/essentialmedicines/EML2015_8-May-15.pdf
- ↑ Fluvoxamine | https://www.drugs.com/cdi/fluvoxamine.html
- ↑ Hashimoto, K. (September 2009). "Sigma-1 receptors and selective serotonin reuptake inhibitors: clinical implications of their relationship". Central Nervous System Agents in Medicinal Chemistry. 9 (3): 197–204. doi:10.2174/1871524910909030197. ISSN 1875-6166.
- ↑ Paroxetine | https://www.drugs.com/paroxetine.html
- ↑ Sertraline | https://www.drugs.com/sertraline.html
- ↑ Owens, J. M., Knight, D. L., Nemeroff, C. B. (August 2002). "[Second generation SSRIS: human monoamine transporter binding profile of escitalopram and R-fluoxetine]". L’Encephale. 28 (4): 350–355. ISSN 0013-7006.
g