Serotonin
This article is a stub. As such, it may contain incomplete or wrong information. You can help by expanding it. |
Serotonin (also known as 5-hydroxytryptamine, or 5-HT), is a naturally occuring chemical found in humans, animals, and plants alike.
It exerts its effects through the monoamine neurotransmitters affecting the 14 known serotonin receptors (5-HT1A,1E,1F, 5-HT1Dα,1Dβ, 5-HT3,4,6,7, 5-HT2A,2B,2C, 5-HT5A-5B)[1] 90%-95% of serotonin is located in the gastrointestinal tract, in blood platelets 8% and in the central nervous system 1%-2%.[2]
It is commonly referred to as one of many "happy hormones" amongst dopamine, oxytocin, and endorphins, these chemicals bring about feelings of happiness and wellbeing (although this is a major oversimplification).
Approximately 95% of the human body's serotonin is produced in the intestines, where it has been credited with effects related to hormonal, autocrine, paracrine, and endocrine actions. [3] What is not absorbed elsewhere in the body is synthesized into serotonergic neurons for use by the central nervous system or CNS, here the serotonergic neurons can regulate: sleep, appetite, sexual behavior, homeostasis/temperature regulation, pain, and cognition.
Serotonin also affects pathological states such as: disorders connected to mood, anxiety, psychosis and pain.[4] Having either too little or too much serotonin can have many negative effects.
In the blood, it serves as a vasoconstrictor, and could be attributed as the cause of vasoconstriction in most serotonergic drugs.[citation needed]
Chemistry
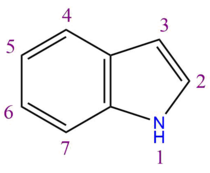
Serotonin is comprised of a monoamine chain attached to an indole ring at the third carbon. A monoamine chain is made up of an amine group attached to an ethane chain.
This monoamine chain can be found in many neurotransmitters, including histamine, dopamine, adrenaline and noradrenaline. It is also found in many drugs, e.g. tryptamines and phenethylamines.
Serotonin is synthesized from the α-amino acid tryptophan, which is hydroxylated into the metabolic intermediate 5-Hydroxytryptophan (5-HTP) and then decarboxylated into serotonin. This process requires the co-enzyme vitamin B6.[citation needed]
Serotonin system
This article is a stub. As such, it may contain incomplete or wrong information. You can help by expanding it. |
The serotonin receptor, or 5-HT receptors, are found throughout the central nervous system and the peripheral nervous system.
Drugs targeting the 5-HT system
Full agonists
A serotonin full agonist is a chemical that binds to and activates a serotonin receptor and triggers a response, displaying full efficacy at that receptor.
A few psychedelic drugs are full agonists of the 5-HT2A receptor; among them are 25I-NBOMe and Bromo-DragonFLY.
Partial agonists
A serotonin partial agonist is a drug that binds to and activates a serotonin receptor, but only has partial efficacy at the receptor relative to a full agonist.
Most classical psychedelic drugs are partial agonists of the 5-HT2A receptor; among them are LSD, psilocin and mescaline.
Many antidepressants, anxiolytics/anti-anxiety drugs, and cluster headache medicines are partial serotonin receptor agonists.
Inverse agonists
A serotonin inverse agonist activates a serotonin receptor but has the opposite pharmacological effect. Inverse agonists trigger a specific response from a receptor, whereas antagonists inhibit the activity of the receptor.
Some antipsychotics such as Pimavanserin, Risperidone and Olanzapine are 5-HT2A inverse agonists. 5-HT2A inverse agonists have been researched for the treatment of insomnia with limited success.
Releasing agents
A serotonin releasing agent is a drug that induces the release of serotonin from the presynaptic neuron into the synapse, leading to an increase in the extracellular concentrations of serotonin.
Many recreational drugs are serotonin releasing agents; among them are MDMA, MDA and mephedrone. Many analgesics/pain-relievers and appetite suppressants are also serotonin releasing agents.
Reuptake inhibitor
A serotonin reuptake inhibitor inhibits the reabsorption of serotonin into the pre-synaptic neuron. Serotonin reuptake inhibitors do this by inhibiting the serotonin transporter, or SERT protein.
Many antidepressants such as: venlafaxine (Effexor), an SNRI, citalopram (Celexa), a SSRI and amitriptyline (Elavil), a TCA these antidepressants all exert there action through serotonin reuptake inhibitors. Many recreational drugs like cocaine and tramadol are also serotonin reuptake inhibitors.
Antagonists
A serotonin receptor antagonist is a type of receptor drug that inhibits action at serotonin receptors.
Many antipsychotics such as, haloperidol or quetiapine and anti-emetics are serotonin receptor antagonists. One example is galanolactone, a chemical found in ginger, that acts as an anti-emetic via its action as a 5-HT3 antagonist.
Toxicity and harm potential
 |
This toxicity and harm potential section is a stub. As a result, it may contain incomplete or even dangerously wrong information! You can help by expanding upon or correcting it. |
Serotonin syndrome
Extremely high levels of serotonin can cause a condition known as serotonin syndrome, which possess both toxic and potentially life threatening effects.
Serotonin syndrome, also known as serotonin toxicity, is not known to occur naturally without the introduction of a pharmaceutical or supplemental agent. However, serotonin syndrome is known to develop from naturally occurring compounds such as St. John's Wort, a treatment for depression, due to its similarities to already existing antidepressants. Excess amounts of serotonin in the brain is primarily caused by the concurrent use of two or more serotonin acting drugs.[5]
An example that may result in serotonin syndrome would include taking two antidepressants in combination such as Escitalopram (Lexapro) with Duloxetine (Cymbalta), since both drugs act on some of the same receptors they may cause serotonin syndrome.
Another example would be taking a prescription antidepressant in combination with an over the counter cough suppressant such as dextromethorphan.[6][7]The number of possibly dangerous combinations are numerous. If you are currently taking an antidepressant or are considering taking a new substance, ensure that no dangerous interactions exist.
Symptoms can start showing within hours and can include: increased or irregular heart rate, tremors, low-grade fever to fevers at or over 41°C (105.8°F), sweating, anxiety, hyperthermia, shivering, high blood pressure, restlessness, dilation of the pupils, overactive or over responsive reflexes, agitation, confusion, death of muscle fibers, clotting of small blood vessels, increase in body acidity, delirium, renal (kidney) failure, coma and rarely death.[8]
Symptoms in minor cases may resolves within days, moderate cases may resolve within weeks, and in severe cases permanent damage or death may occur.
See also
External links
- Serotonin (Wikipedia)
- Tryptophan (Wikipedia)
- 5-Hydroxytryptophan (Wikipedia)
- Serotonin (Isomer Design)
Literature
- Sodhi, M., & Sanders-Bush, E. (2004). Serotonin and brain development. International Review of Neurobiology, 59, 111-74. https://doi.org/10.1016/S0074-7742(04)59006-2
- Nichols, D.E., & Nichols, C.D. (2008). Serotonin receptors. Chemical Reviews, 108 5, 1614-41. https://doi.org/10.1021/cr078224o
- Berger, M., Gray, J.A., & Roth, B.L. (2009). The expanded biology of serotonin. Annual Review of Medicine, 60, 355-66. https://doi.org/10.1146/annurev.med.60.042307.110802
- Aghajanian, G., & Marek, G. (1999). Serotonin and Hallucinogens. Neuropsychopharmacology, 21, 16S-23S. https://doi.org/10.1016/S0893-133X(98)00135-3
References
- ↑ Frazer, A., Hensler, J. G. (1999). Siegel, G. J., ed. “Serotonin”. Basic neurochemistry: molecular, cellular, and medical aspects (6th ed ed.). Lippincott Williams & Wilkins. ISBN 9780397518203.
- ↑ Kling, A. (2013). 5-HT2A a serotonin receptor with a possible role in joint diseases. Ume Universitet. ISBN 9789174595499.
- ↑ Terry, N., Margolis, K. G. (2017). "Gastrointestinal Pharmacology". In Greenwood-Van Meerveld, B. Serotonergic Mechanisms Regulating the GI Tract: Experimental Evidence and Therapeutic Relevance. Handbook of Experimental Pharmacology. Springer International Publishing. pp. 319–342. doi:10.1007/164_2016_103. ISBN 9783319563602.
- ↑ Chilmonczyk, Z., Bojarski, A., Pilc, A., Sylte, I. (7 August 2015). "Functional Selectivity and Antidepressant Activity of Serotonin 1A Receptor Ligands". International Journal of Molecular Sciences. 16 (8): 18474–18506. doi:10.3390/ijms160818474. ISSN 1422-0067.
- ↑ Lane, R., Baldwin, D. (June 1997). "Selective Serotonin Reuptake Inhibitor-Induced Serotonin Syndrome: Review". Journal of Clinical Psychopharmacology. 17 (3): 208–221. doi:10.1097/00004714-199706000-00012. ISSN 0271-0749.
- ↑ Monte, A. A., Chuang, R., Bodmer, M. (December 2010). "Dextromethorphan, chlorphenamine and serotonin toxicity: case report and systematic literature review: Dextromethorphan, chlorphenamine and serotonin toxicity". British Journal of Clinical Pharmacology. 70 (6): 794–798. doi:10.1111/j.1365-2125.2010.03747.x. ISSN 0306-5251.
- ↑ Schwartz, A. R., Pizon, A. F., Brooks, D. E. (January 2008). "Dextromethorphan-induced serotonin syndrome". Clinical Toxicology. 46 (8): 771–773. doi:10.1080/15563650701668625. ISSN 1556-3650.
- ↑ Frank, C. (1 July 2008). "Recognition and treatment of serotonin syndrome". Canadian Family Physician. 54 (7): 988–992. ISSN 0008-350X.