Talk:Extrapyramidal symptoms
Extrapyramidal symptoms (EPS), also known as extrapyramidal side effects (EPSE), are drug-induced movement disorders that include acute and tardive/chronic symptoms. They are mainly caused by the blockade of dopamine at dopaminergic receptors.
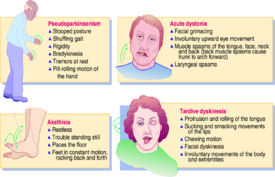
Types and their symptoms
Acute dystonia
Acute dystonia is a painful and often severe type of extrapyramidal symptoms that occurs shortly (within less than a day)[citation needed] after the administration of an antidopaminergic agent.
Continuous muscle contractions can occur in the head, neck, and limbs and may cause a stiff tongue, arched back, or twisted neck. Dystonia also includes a lack of ability to move muscle and low muscle tone.
Treatment of acute dystonia is often an anticholinergic agent and/or a benzodiazepine.[citation needed]
Akathisia
Akathisia is characterized by restlessness, a need to move, constant sitting down and standing up, pacing, etc. Treatments for akathisia are anticholinergics, beta blockers, or benzodiazepines. Akathisia typically develops some time during a medication regimen[citation needed]
Psuedoparkinsonism
Psuedoparkinsonism occurs often further than akathisia.[citation needed] It is often noticed by seeing:
- tremoring hands in a "pill-rolling" pose,
- a stooped posture,
- slowed movements,
- shuffling, small steps,
and others. Others also include that when the person turns, they must do so very slowly and sometimes cannot change positions, such as standing to sitting, without a support.
Tardive dyskinesia
This disorder develops over long periods of time[citation needed] and is noticed by these signs: involuntary chewing, lip smacking or sucking, twitching, and/or involuntary movements of the limbs that are often jerky. It is treated by putting the patient on a dopaminergic medication regimen, such as using valbenzaine, tetrabenazine, ropinirole, or pramipexole.
Causes
Extrapyramidal symptoms are most commonly caused by typical antipsychotic drugs that antagonize dopamine D2 receptors. The most common typical antipsychotics associated with EPS are haloperidol and fluphenazine.[1]
Other antidopaminergic drugs, like the antiemetic metoclopramide, can also result in extrapyramidal side effects.[2]
Short and long-term use of antidepressants, such as selective serotonin reuptake inhibitors (SSRI), serotonin-norepinephrine reuptake inhibitors (SNRI), and norepinephrine-dopamine reuptake inhibitors (NDRI) has also resulted in extrapyramidal symptoms. Specifically, duloxetine, sertraline, escitalopram, fluoxetine, and bupropion have been linked to the induction of extrapyramidal symptoms.[3]
Treatment
Anticholinergic drugs are used to control neuroleptic-induced EPS, although akathisia may require beta blockers or even benzodiazepines. If the EPS are induced by an antipsychotic, EPS may be reduced by dose titration or by switching to an atypical antipsychotic, such as aripiprazole, ziprasidone, quetiapine, olanzapine, risperidone, or clozapine.
Commonly used medications for EPS are anticholinergic agents such as benztropine (Cogentin), biperiden (Akineton), diphenhydramine (Benadryl), and trihexyphenidyl (Artane). Another common course of treatment includes dopamine agonist agents, such as pramipexole and ropinirole. These medications reverse the symptoms of extrapyramidal side effects caused by antipsychotics or other drugs that either directly or indirectly inhibit dopaminergic neurotransmission.
Literature
External links
Extrapyramidal symptoms (Wikipedia)
See also
- Antipsychotics
- Haloperidol, one of the most common agents associated with EPS
- Risperidone, another agent known to induce EPS
- Diphenhydramine, an agent sometimes used to treat EPS
- Responsible drug use
- Dopamine
References
- ↑ Note, I. (2009). Extrapyramidal adverse effects. Biomed Res Int., 2014, 30–32. https://doi.org/10.1155/2014/656370
- ↑ Moos, D. D., & Hansen, D. J. (2008). Metoclopramide and Extrapyramidal Symptoms: A Case Report. Journal of Perianesthesia Nursing, 23(5), 292–299. https://doi.org/10.1016/j.jopan.2008.07.006
- ↑ Madhusoodanan, S., Alexeenko, L., Sanders, R., & Brenner, R. (2010). Extrapyramidal symptoms associated with antidepressants--a review of the literature and an analysis of spontaneous reports. Annals of Clinical Psychiatry : Official Journal of the American Academy of Clinical Psychiatrists, 22(3), 148–56. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/20680187